Knowing about your sexual and reproductive anatomy and understanding how your body works is an important part of sexual health. It can help you:
- Understand what’s going on with your body and get to know what’s normal for you.
- Ask questions about what’s happening with your body.
- Tell other people about what’s happening with your body or what you want to happen, like how you do and don’t want to be touched.
- Get and understand information about pleasure, sex, pregnancy, birth control, STIs, or other topics.
- Recognize when something is not normal for you and/or when you might need to get sexual health care.
Note: We have used words for body parts that you may not use or relate to in the same way. We have used these words as they are commonly known and encourage you to use the language that feels best for you.
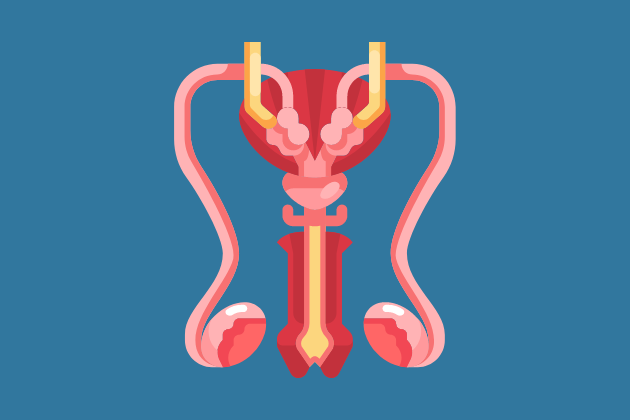
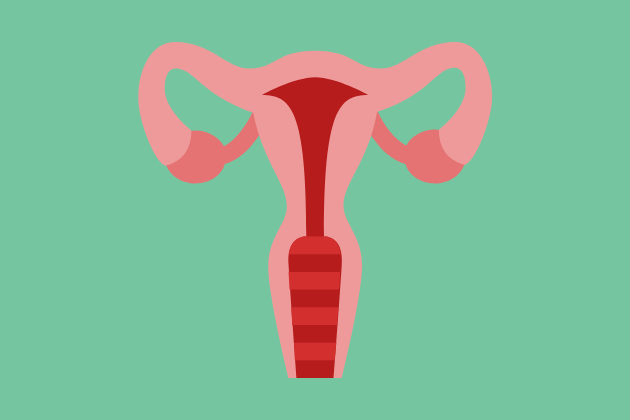
Your Body Parts
Knowing the names of your (and other people’s) body parts and what they do can be a great starting point for learning and talking about sexual health. These pages have information about the internal and external parts of the genitals and what they do.
How Your Body Works
Bodies aren’t just parts: they’re systems, and talking about sexual health means talking about the processes those systems go through. Learning about those processes can help you understand what’s happening in your body, talk about it with other people, and get healthcare if you need it.